Eliquis (generic name apixaban) is commonly used as an anticoagulant for the treatment of:
- Deep vein thrombosis
- Pulmonary embolism
- blood clots resulting from atrial fibrillation resulting in strokes
- Recurrence of pulmonary embolism or DVT
In a 2018 study of the effectiveness of the classes of drugs being used in treating Atrial Fibrillation cases, Eliquis was declared to be the safest for stroke prevention.
In the United States, Eliquis is also approved to treat deep vein thrombosis and pulmonary embolism and as a longer-term medication to prevent them from reforming.
What are some of the conditions where blood thinners are needed?
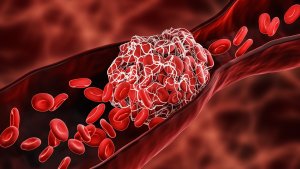
There are many conditions resulting in blood clotting that can potentially lead to serious outcomes. In general, the dangers that blood clots can lead to range from risk of stroke resulting in partial paralysis, all the way through to systemic embolism that can be fatal. The usual therapy to prevent clotting is taking anticoagulants, which act as blood thinners that reduce the chance of blood clotting. Eliquis is one of the most frequently prescribed anticoagulants.
Primer – what causes blood to clot?
Clotting, properly called coagulation, is an essential and natural function of the blood. For example when you scratch your knee and it starts to bleed, usually as soon as it comes into contact with the air, it will start to coagulate and the flow of blood will slow and stop, finally forming a scab so that the injury can heal underneath.
If you want to know more about this subject, there’s a great explanation on the bleedingdisorders.com website.
However, coagulation inside the vessels carrying blood around the body can prove to be highly dangerous. Blood clots can grow in size until they form a large body, known as a thrombosis. This can cause blockages to the flow of blood through arteries and veins, resulting in damage to the tissues further down the network due to oxygen deprivation and resulting in cell death.
What conditions causing blood clotting do direct oral anticoagulants (DOACs) treat?
- Atrial fibrillation, which shows up as an irregular and rapid heartbeat
- Deep Vein Thrombosis after knee or hip replacement surgery.
Atrial Fibrillation (AF)
The usual cause of AF is where one or more heart muscles are not beating as they should. Atrial fibrillation is the most common serious abnormal heart rhythm. It was reported last year that it affects more than 33 million people worldwide.
Atrial fibrillation may occur in otherwise normal hearts, but much more often is linked to cardiovascular disease, including high blood pressure, coronary artery disease, rheumatic heart disease or mitral valve prolapse and left atrial enlargement. Some congenital heart diseases also manifest as atrial fibrillation, and people with a family history of the condition among first-degree relatives run a 40% increase in the risk of AF.
Several other general health changes can cause AF, mainly heart surgery or a heart attack.
How does Atrial Fibrillation cause clotting?
Often, changes are seen in blood vessel walls, in flow volume and in blood constituents that in combination contribute to thrombus formation (technically known as thrombogenesis) in atrial fibrillation. These abnormal changes may take place in one or more of the promoters of clotting, that seem to be unrelated to the cause of atrial fibrillation.
What are the common treatments for Atrial Fibrillation?
Treatment takes three primary forms:
- Lifestyle changes
- Cardiac rhythm modulation
- Anticoagulants
Lifestyle modification
Many of the causes of AF are related to lifestyle and general health. These include obesity, high blood cholesterol, smoking, and alcohol consumption. Doctors recommend addressing these issues along with any other treatments.
Modification of the heart’s rhythm
Initially, most treatments try to restore a normal heart rhythm with a single electrical or chemical “jolt” (known as cardioversion) and maintain the rhythm with drugs.
Electrical cardioversion delivers an electrical shock to the heart, which briefly stops the heart’s electrical activity for a few seconds. The object is for it to resume with normal rhythm.
Cardioversion with drugs uses medications to help restore normal rhythm.
Post-cardioversion, doctors usually prescribed medications called antiarrhythmics to help prevent future episodes of atrial fibrillation.
Anticoagulation
The danger coming from AF is of a thrombosis leading to a blockage that may cause a stroke or heart attack. Anticoagulants are usually recommended in most people other than those at high risk of bleeding.
The general classification of this type of drug is a direct oral anticoagulant (DOAC). You can read more about these further down.
Can direct oral anticoagulants help with deep vein thrombosis (DVT) after knee and hip replacement?
Deep vein thrombosis (DVT) is a serious condition in which a blood clot that developed in a vein can break away and cause a number of potentially fatal results. The clot could travel to the lungs and cause a pulmonary embolism.
The blood clots related to DVT most frequently develop in the legs and may cause the post-thrombotic syndrome, which manifests as swelling and pain. If untreated, it can result in permanent damage to the legs.
Because DVT most frequently develops in the lower part of the body, patients who have had hip or knee replacement surgery are at greater risk of serious side effects from DVT. Research has shown that the risk period for clots in the deep veins can be up to 12 weeks after hip replacement and up to six weeks after knee surgery.
Post-surgery, patients are usually advised to take some steps to minimize the chance of DVT developing, including:
- Exercise and movement to stimulate blood circulation around the affected limb to prevent clots from forming
- Fitting a special pneumatic sleeve on the legs that keeps blood moving
- Wearing special compression stockings to promote circulation and minimize swelling
- Taking prescribed anticoagulants.
Tell me more about direct oral anticoagulants
For many years, the anticoagulants most frequently prescribed for patients were aspirin or warfarin. Currently, there have been numerous studies that show that the DOAC class of drugs such as rivaroxaban, edoxaban, and apixaban offer significant benefits. The speed of the desired onset of anticoagulation makes DOACs at least as effective as warfarin for preventing strokes and blood clots, if not more so. DOACs carry a lower risk of bleeding in the brain compared to warfarin.
Tell me more about Eliquis
Eliquis’ main therapeutic ingredient is the DOAC apixaban, which works as an anticoagulant to block specific clotting proteins in the blood.
According to a published report, in a 2018 follow-up of the effectiveness of DOAC drugs in treating AF cases, Eliquis was declared to be the safest effective DOAC for stroke prevention in AF, as per the Agency for Healthcare Research and Quality’s (AHRQ) report.
In the United States, Eliquis is also approved to treat deep vein thrombosis and pulmonary embolism and as a longer-term medication to prevent them from reforming.
What are common side effects and contraindications of direct oral anticoagulants like Eliquis?
Among the more common mild side effects are nausea, easy bruising, or minor spontaneous bleeding such as a nosebleed or bleeding from scrapes and cuts that don’t stop quickly.
Although severe side effects are extremely rare, be sure to tell your healthcare provider or pharmacist if you experience any feelings of discomfort, or, most importantly, severe spontaneous bleeding.
Be sure to tell your doctor or pharmacist immediately if you have any of the following symptoms:
- serious bleeding
- coughing up blood
- unusually heavy or prolonged menstrual flow
- unusual pain, swelling, discomfort or bruising
- prolonged bleeding from cuts or gums
- persistent/frequent nosebleeds
- pink/dark urine
- severe headache
- dizziness or fainting
- unusual or persistent tiredness or weakness
- bloody/black/tarry stools, or dark-colored vomiting
Your doctor will have given proper consideration to how the active ingredients in Eliquis interact with your other medications and could affect your health. In all cases, the doctor will consider that any adverse effects will be far outweighed by the life-giving benefits that Eliqis brings to patients with your condition. If you are in any doubt, discuss this with your doctor and pharmacist.
What is the recommended dosage of Eliquis?
Your doctor will prescribe the dosage that is appropriate to your condition, as well as factors such as age, body weight and more.
Take the medication according to the instructions you receive from your dispensing pharmacist, and the enclosed pamphlet you receive.
Important: Do not take Eliquis with any form of alcohol.