The sudden arrival of COVID-19 at the start of 2020 broke an established pattern of how the influenza virus swept through countries with the onset of winter. Until then, it was reasonably well understood that each year saw a slightly new variant of the virus, but there was enough knowledge for scientists to be able to build a vaccine each year that could provide a good degree of protection, if not to actual infection, but to serious rates of hospitalization and morbidity.
One of the side benefits of this successful immunization program was that the general population was building up a higher level of natural immunity to influenza. This was since they had been able to fight off a longer string of different flu variants, which meant there were more triggers in their immune systems to recognize most variants quickly and start fighting them without medication.
The COVID-19 pandemic years threw this pattern into disarray. In 2020 and 2021, the battle against the coronavirus took precedence. There were self-isolation, mask-wearing and work-from-home programs removing a large proportion of the population from physical mingling, so influenza rates dropped dramatically.
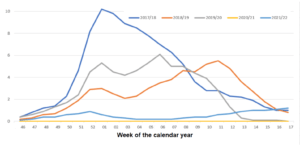
The following graph we generated from data drawn from the government’s FluView website draws a clear picture. It shows a weekly count of flu cases in the US for the last five years, from November through to the following April. These are the winter months when influenza infections have historically peaked. (https://thecenturionreport.com)
Prior to the onset of the coronavirus pandemic, the numbers climbed and stayed high until around late March. In the winter of 20/21, when the pandemic was raging, people stayed at home, washed their hands, used sanitizers and took other precautions as much as possible. The numbers of flu cases were so low that they couldn’t even be rated compared to the millions in prior years. Only in 21/22, once the COVID-19 pandemic had come to be at least manageable, if not defeated, did flu numbers start to climb to anything near the levels of previous years. A final observation – this year, flu numbers in the current summer months are actually higher than any recorded during the last twenty years. Could this be a precursor to what the story unfolding in Southern hemisphere countries like Australia is telling us?
The 2022 Australian winter is a “perfect storm,” a “twindemic of covid and influenza.”
We have all, unfortunately, had to become familiar with the term “pandemic”. Now there is a picture coming out of the Southern Hemisphere telling us that the word doesn’t only relate to COVID-19 but also to the older and more established waves of influenza that hit every winter. These two are coming in sync for the first time, so the term “twindemic” has been invented to paint a picture of how much things are changing from established patterns in the coming year.
Australia has an alarming wave of flu case rates that have eclipsed those in the pre-pandemic years. Since the start of winter in May, the weekly number of confirmed cases has exceeded the five-year average, and COVID-19 cases triggered by the Omicron variants are spreading alarmingly.
Some features of the spread of influenza in Australia this year add to the concerns. Usually, flu cases start to build up in June, when the cold and wet begin to bite in the populous southern states of Victoria and New South Wales.
This year, cases started to spike as early as April, and already the massive numbers, only halfway through winter, suggest that new flu strains are circulating in the Southern Hemisphere. Australia has also seen more than 47,000 new coronavirus cases daily since February, mainly due to Omicron variants. Hence the fear that there’s a twindemic playing out down under.
What does this twindemic mean for the US?
One of the first fallouts of the Australian experience is that it throws the whole influenza vaccine program for the US into disarray. For many years, developing a new vaccine each year for the Northern Hemisphere countries has been mainly based on vaccination results in Australia and New Zealand. Now, there is far less reliable data from their vaccination programs, which puts the effectiveness of the US’s own vaccination into doubt.
Suppose another significant COVID-19 variant comes along and the flu season follows without an effective vaccine having been widely distributed. In that case, there’s no telling what the outcome could be. The US population may now face the same possibility of a twindemic as Australia.
What are the possible remedial steps?
Americans have developed “vaccine fatigue” over the past year. As a result, they may decide to skip both the standard influenza vaccine and any of the new COVID-19 mRNA vaccine boosters targeting the BA.5 and Omicron variants. This will put them at serious risk of contracting both flu and covid and of infecting people around them.
Federal and state health authorities should pull out all the stops, including offering some financial incentives, to get the population to roll up their sleeves and get the jabs.